Treatment for Nail Psoriasis; Why You Don't Have to Hide Nail Psoriasis Anymore!

Treatment for nail psoriasis is frustrating. Psoriasis of the finger and toenails is disfiguring and potentially uncomfortable so it is exciting to have new treatment guidelines.
New treatment guidelines for nail psoriasis
 New treatment guidelines were just released by the Medical Board of the National Psoriasis Foundation and published in JAMA Dermatology. If you or someone you know has psoriatic nail problems, you’ll want to be aware of this paper.
New treatment guidelines were just released by the Medical Board of the National Psoriasis Foundation and published in JAMA Dermatology. If you or someone you know has psoriatic nail problems, you’ll want to be aware of this paper.
What happens to nails when you have psoriasis?
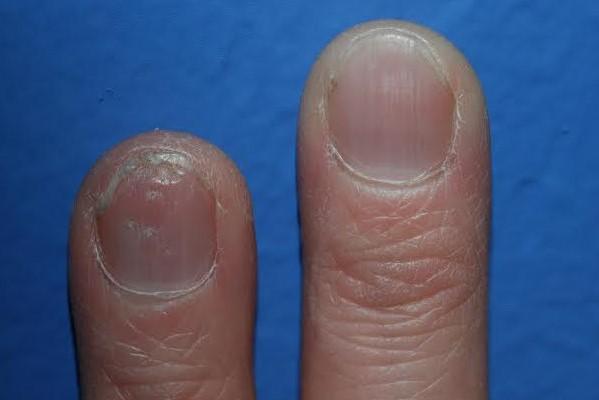
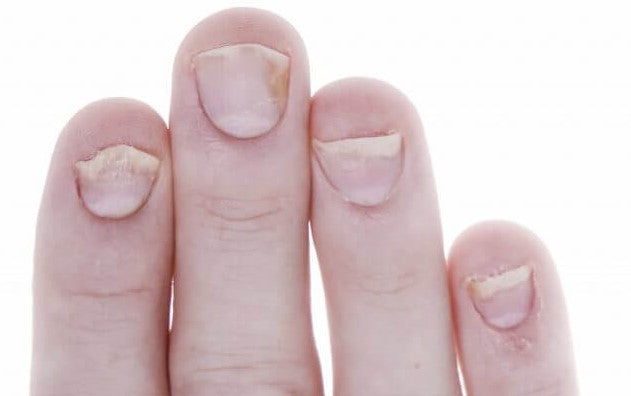 Nails become thick, deformed, and pitted and lift off the skin. As you can imagine, thickened and deformed nails can be painful. Nail fungus loves to live in these sort of nail deformities, which give the infecting fungi and molds a "toe hold" (cheeky pun) and adds to the problem. About 50% of people with psoriasis also have nail psoriasis at any one time. If you have psoriasis, you have an 80% to 90% chance of suffering these nail problems at some point in your lifetime. Unfortunately, treatment is really frustrating and very little has worked in the past to control nail psoriasis.
Nails become thick, deformed, and pitted and lift off the skin. As you can imagine, thickened and deformed nails can be painful. Nail fungus loves to live in these sort of nail deformities, which give the infecting fungi and molds a "toe hold" (cheeky pun) and adds to the problem. About 50% of people with psoriasis also have nail psoriasis at any one time. If you have psoriasis, you have an 80% to 90% chance of suffering these nail problems at some point in your lifetime. Unfortunately, treatment is really frustrating and very little has worked in the past to control nail psoriasis.
What’s new in the National Psoriasis Foundation recommendations?
There are four scenarios with treatment recommendations described in the article. The bottom line is that treatment persistence pays off!
Nail Psoriasis Treatment Scenario #1: There are 3 to 10 nails involved with minimal pain.
They recommend high-powered topical cortisone medicines or cortisone combined with calcipotriol. Injections of cortisone into the nail can also be done (ouch!).
Nail Psoriasis Treatment Scenario #2: 5 to 10 nails are involved with no pain and no skin or joint involvement.
If the topical care, as described in Scenario #1, doesn't work, then they recommend systemic treatment with either adalimumab, etanercept, intralesional corticosteroids, ustekinumab, methotrexate, or acitretin, in that order.
Nail Psoriasis Treatment Scenario #3: 5 to 10 nails are involved with moderate pain or more and at least 8% of the body skin is affected by psoriasis.
If topical treatment has failed, then they recommend adalimumab, etanercept, and ustekinumab as their first-choice options and methotrexate, acitretin, infliximab, and apremilast as alternatives.
Scenario #4: Skin, joint, and nail disease are significant, meaning 5 to 10 nails are severely involved and there is a lot of discomfort. About 8% of the body’s skin has psoriasis and there is some arthritis and morning stiffness.
In this scenario, they recommend these internal medicines from first choice to lowest choice: adalimumab, etanercept, ustekinumab, infliximab, methotrexate, apremilast, and golimuma. With systemic treatments of psoriasis, it’s important to know that skin and joint problems respond faster than problems in the nails. This means it can take 12 weeks or more to see any changes in the nails, but they do happen.
Remember, too, that psoriasis is a systemic disease linked to other health problems - it's not just a skin and nail disease. The really good news about psoriasis is that is also responds to lifestyle interventions.
The same healthy diet and exercise that’s good for your heart and lowers your risk of cancer or diabetes will improve your psoriasis.
I always recommend a whole-body approach to psoriasis treatment that involves diet and lifestyle along with skin care and prescription medicines.
What are the recommendations I give to my psoriasis patients in my dermatology practice?
Find it here in these articles that I have written:
- Skin Care Tips to Heal Psoriasis
- Lifestyle Changes to Help Heal Psoriasis
- Health Concerns Related to Psoriasis
If you found this information helpful, sign up for my free newsletter; get your skin care and skin health information from a dermatologist!
Please share this post with anyone you know that has psoriasis - it's a frustrating condition, but this news gives hope!
References:
Crowley JJ, Weinberg JM, Wu JJ, et al. Treatment of nail psoriasis: best practice recommendations from the Medical Board of the National Psoriasis Foundation. JAMA Dermatol. 2015;151:87-94.
