Autoimmune Diseases and Your Skin

Autoimmune diseases and your skin often provide an early sign that your immune system is not working correctly. Skin is your body's biggest organ and it makes sense that autoimmune disease will cause changes on your skin. Normally, when the immune system works well, your complicated immune system attack things that are harmful, foreign and that your body needs to protect you from. This includes things such as viruses and bacteria.
When your body attacks normal and healthy parts of itself, we call the result an autoimmune disease; your immune system sees your normal and healthy cells and tissue as foreign invaders and attacks them. Your immune system may see cells in your skin as foreign and the attack shows up as a rash on the skin. It can attack other organs and/or your joints, and the process can lead to generalized inflammation.
Autoimmune Diseases and Your Skin
- How do autoimmune diseases happen?
- What are the most common autoimmune diseases and which are most likely to show skin changes?
- Lupus is an important autoimmune disease that often first shows up first as a skin problem
- How does a person know if they have the autoimmune disease systemic lupus?
- For those that do have lupus, one of the most important practices to prevent flare-ups of the disease is meticulous sun protection
The common theme between all autoimmune diseases is inflammation. Some autoimmune diseases restrict themselves to certain organs (for example, Graves’ disease, which for the most part, is a disease that only attacks the thyroid). Other diseases like lupus can affect almost any part of the body. Inflammation that is organ specific, like Graves, or more generalized, like lupus, can also cause abnormal inflammation in the body as a whole. Autoimmune diseases are complex, your skin is large and visible, and it is common to see skin changes when you have an autoimmune disease.
How do autoimmune diseases happen?
We don’t completely understand why autoimmune diseases occur. Some people are genetically predisposed to these diseases and some ethnic groups are more prone to certain autoimmune diseases. It’s also possible that an outside influence like a virus or other infection may trigger the onset of autoimmune disease.
Where does dermatology fit into autoimmune diseases?
Dermatologists evaluate and treat autoimmune diseases as part of their practice. The skin is a big and visible organ and often the 'tip of the iceberg' for an autoimmune disease. Often, we are the first to make a diagnosis that then also needs treatment and care by general physicians and rheumatologists who treat the internal consequences of a misfiring immune system.
Certain autoimmune diseases have classic skin manifestations and we are trained to recognize them.
The most common autoimmune diseases and your skin risk of developing rashes from them.
Some of the more common autoimmune diseases are listed here. I've bolded the autoimmune conditions that often present first as a skin problem.
- Alopecia areata
- Autoimmune hemolytic anemia
- Autoimmune hepatitis
- Dermatomyositis
- Diabetes (type 1)
- Graves’ disease
- Guillain-Barré syndrome
- Idiopathic thrombocytopenic purpura
- Myasthenia gravis
- Some forms of myocarditis
- Multiple sclerosis
- Lupus erythematosus
- Scleroderma
- Vitiligo
- Bullous pemphigoid
- Pemphigus vulgaris
- Granulomatosis with polyangiitis
- Polyarteritis nodosa
- Rheumatoid arthritis
- Lichen Planus
Lupus is an important autoimmune disease and you skin may be the first sign.
One of the more common symptoms of lupus is a photosensitive skin rash. The skin is "allergic" to the sun and when a person with lupus goes out into the sun, they feel sick and develop a rash. One of the rashes of lupus is the “malar” (butterfly) rash that covers the cheeks and nose.
The sun can trigger both a rash and a flare-up of the disease inside the body too. The malar rash is a warning sign that the disease is active. The rash of lupus is important to recognize because, when lupus is untreated, it has the potential to cause damage to other organs such as the kidneys, lungs or heart. We call this systemic lupus and it can affect almost any organ.
Other skin findings with systemic lupus are ragged cuticles and tiny dilated blood vessels around the edge of the cuticles. It seems like a small thing to worry about but it can indicate a bigger autoimmune problem inside of the body.
Lupus rashes can also occur on any area that is exposed to the sun. Sun sensitivity is important to take seriously because skin problems may be one of the first symptoms of systemic lupus.
Another type of lupus is called subacute cutaneous lupus. It doesn’t typically have internal involvement but it does cause sun-sensitive rashes.
A dermatologist will do a skin biopsy to look for lupus if sun sensitivity and a rash is suspicious for this diagnosis.
How does a person know if they have the autoimmune disease systemic lupus?
The diagnosis is made when a person meets a certain number of diagnostic criteria. One needs to have 4 of the following problems to be diagnosed with lupus:
- Skin rashes: either a malar rash, discoid rash (somewhat circular-shaped scarring skin lesions) or a rash on sun-exposed areas
- Mouth sores
- Arthritis
- Pleurisy (inflammation of the lungs) or pericarditis (inflammation of the heart)
- Abnormal blood tests such as low white blood cell counts or platelets
- Kidney problems consistent with lupus
- Neurologic problems such as psychosis or seizures that can happen due to inflammation in the brain
- Abnormal autoantibody tests such as a positive ANA (anti-nuclear antibody test); almost all patients with lupus have a positive ANA. However, many people without lupus have a positive ANA as well so it’s important for this to be interpreted by a rheumatologist.
For those that do have lupus, one of the most important practices to prevent flare-ups of the disease is meticulous sun protection.
This is another important role for your dermatologist. Teaching you how to prevent UV ray exposure on your skin is really important for controlling lupus. A really good broad spectrum sunscreen should be used every day on all exposed skin.
- The best sun protection comes from physical mineral sunscreen zinc oxide. Mineral sunscreens are ideal because they are also non-irritating to sensitive skin with an active autoimmune rash.
- Broad spectrum zinc oxide sunscreen with SPF 30 or higher must be applied regardless of whether you plan to go outdoors because UVA rays come through windows and can set off lupus.
In my 35+ years of dermatology practice here in California, I've taken care of many patients with lupus, autoimmune diseases, photosensitivity diseases and predisposition to skin cancer. Together, we've put sun protection to the test.
 Click here to see the sunscreens and sun protection hats and tools that are patient-proven, dermatologist-approved and backed by science.
Click here to see the sunscreens and sun protection hats and tools that are patient-proven, dermatologist-approved and backed by science.

Skin care for lupus
In addition to impeccable sun protection, I always recommend a hypoallergenic and hydrating skin care routine for my patients with complex skin rashes, including those due to autoimmune disease. Lupus in particular can cause rashes that will compromise the skin barrier. You don't want to use anything harsh, irritating or full of taunting allergens on a weakened skin barrier.
-
 Cleanse with gentle fragrance-free products including pH balanced cleansers such as VaniCream Cleansing Bar
Cleanse with gentle fragrance-free products including pH balanced cleansers such as VaniCream Cleansing Bar
-
Apply a fragrance-free deeply hydrating moisturizer such as my Natural Face and Body Lotion within 3 minutes after cleansing skin and toweling off the excess water.

- Keep a good hand cream in a convenient location to moisturize hands after washing many times during the day. My Dry Skin Hand Repair Cream is fragrance-free, non-greasy and the ideal dermatologist-recommended hand cream.
-
 Use a flavor and fragrance-free lip balm to prevent chapped lips such as my Natural Lip Balm. When in the sun, use a mineral SPF lip balm.
Use a flavor and fragrance-free lip balm to prevent chapped lips such as my Natural Lip Balm. When in the sun, use a mineral SPF lip balm. - Every day apply a pure mineral broad spectrum SPF 30+ sunscreen to all exposed skin. Remember that UVA comes through windows and all UV rays can bounce into shade. Use UPF 50 clothing to sun protect as much skin as possible and always wear a UPF 50 sun hat with a 3+ inch full circumference brim when outside. Be sure that your hat also covers the top of your head.
What are the two most common autoimmune skin diseases?
There are many ways that autoimmune conditions can cause skin problems. The two most common that we see in the dermatology office are:
- Alopecia areata
- Vitiligo
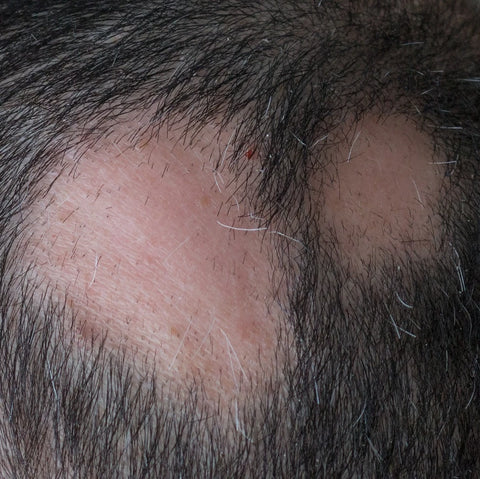
What is alopecia areata?
Alopecia areata is an autoimmune disease where your immune system attacks the hair follicle. This results in clean and clear patches of hair loss. There is no skin scarring and the hair follicles are not damaged. They just don't make hair until the process stops.
Alopecia areata usually targets colored hairs rather than gray hairs.
The hair may grow back white instead of the original hair color at first. Any hair-bearing area can be affected by this condition including eyebrows and eyelashes.
Some people have only a rare patch and mild involvement. Others may have dramatic and/or complete hair loss of the entire scalp, face and body called alopecia universalis.
Alopecia areata is capricious, often behaving unpredictably. Many people with alopecia areata feel that their hair loss worsens when they are under stress.
Alopecia areata may also cause nail problems.
Nail changes that you may see if you have alopecia areata are little pits on the top of the nail.
Alopecia areata can run in families
It can also be related to other autoimmune conditions, namely vitiligo, thyroid problems or inflammatory bowel disease.
What are treatments for alopecia areata.
The most commonly used treatment are cortisone injections into the skin where active hair loss is occurring. Cortisone helps to lower the immune attack at the skin site. If the hair follicles respond, the hairs to regrow.
There are other topical medicines that can be used to treat alopecia areata including Rogaine. In widespread cases, your doctor may discuss systemic pills that help lower the immune system's attack on the hair follicle growing process. These may include oral steroids (prednisone) or cyclosporine.

What is Vitiligo?
Skin pigment cells, called melanocytes, are the target of the autoimmune attack in vitiligo. Because of the attack, skin melanin pigment is lost. This loss of pigment can occur anywhere on the skin. It may be subtle or dramatic.
What does vitiligo look like?
When the condition is subtle, small white patch develop on the skin. When a person's pigment skin tone is light, the white patches may even be very hard to see. In other cases, vitiligo can be extensive and involve a large percentage of the skin. The darker a person's natural skin color is, the more dramatic the white patches of vitiligo appear.
How can doctors tell how bad vitiligo is?
Dermatologists can examine a patch of de-pigmented skin using a black light (technically called a “Wood’s lamp”) to tell if the skin actually lacks pigment completely or is just lighter than surrounding skin. If it’s truly “de-pigmented,” it will look blue under the light.
Vitiligo and stress
Vitiligo, like many autoimmune conditions, may first start after a major stressful event – either emotional or physical.
Is vitiligo connected to other autoimmune diseases?
Most people with vitiligo are healthy. There are, however, certainly genetic factors related to vitiligo. It is also associated with other autoimmune diseases, especially when it is affects a large amount of skin.
The most common associated autoimmune diseases are
- thyroid problems
- type 1 diabetes.
How do you treat vitiligo?
Treatment of vitiligo can be difficult. We usually start with cortisone creams and ointments, especially if there are only small areas affected. If more extensive, ultraviolet light under the supervision of a dermatologist can be considered. In very extensive cases, people may choose to completely de-pigment their skin so that all of the skin is one color, which is what Michael Jackson is said to have done.
Both alopecia areata and vitiligo are important autoimmune diseases because the skin changes are often disturbing to those who suffer from the conditions. It is best to seek care from an experienced Board Certified Dermatologist.
Lastly, I will discuss two really important autoimmune diseases that have distinctive rashes, scleroderma and dermatomyositis.
What is Scleroderma?
Sclerodermaliterally means "hard skin." For reasons we don’t understand, the immune system takes up a war against the skin or internal organs that leads to abnormal deposits of collagen, a.k.a., scleroderma. It can be a very serious disease if advanced. There are two major forms of scleroderma: localized scleroderma and systemic scleroderma. Localized scleroderma is called morphea and shows up on the skin as hard, waxy-looking areas. Often, there is a violet border around it that signifies it is active. But, this type of scleroderma is not associated with organ problems.
Systemic scleroderma, on the other hand, means that the disease has the potential to "harden" other organ systems. Within this type, there is a "limited" and "diffuse" form. The limited form is called "CREST syndrome," which stands for:
- C: Calcinosis is when calcium deposits happen in the skin.
- R: Raynaud’s: This occurs when the blood vessels on the fingers and toes spontaneously constrict in response to even minor changes in temperature or emotional stress. The skin turns white, then blue and then red. Sometimes these episodes are so severe that they can lead to ulcers or permanent death of some of the skin (gangrene).
- E: Esophageal dysmotility is when people may have trouble swallowing or digesting food.
- S: Sclerodactyly: Over time, due to hardening of the skin – mainly on the hands and feet, the fingers and toes contract and become difficult to use.
- T: Telangiectasias: Broken capillaries cover the skin over time. I see these all the time in people but, in scleroderma, they occur in clusters.
"Diffuse" systemic sclerosis is different than CREST syndrome and can have devastating effects on a wide variety of organs including the heart, lungs, kidneys and digestive system.
What is Dermatomyositis?
Dermatomyositisis an inflammatory autoimmune condition that can impact either children or adults. In most cases, it leads to severe muscle inflammation and muscle weakness. This is almost always accompanied by a rash that is very classic-looking and shows up around the eyes, hands, chest and thighs. It is more pronounced in areas that get sun and has a classic violet-looking color. An uncommon condition associated with this is proximal muscle weakness, meaning weakness in the shoulders and hips.
Children get a specific type of dermatomyositis that can lead to painful calcifications in the muscles that can be extremely debilitating. It impacts adults in a different way that can affect other organs in the body as well. The main worry in adults with this disease is if they also have cancer. For some reason, this autoimmune condition can be a sign of an underlying cancer, so I always make sure people are up-to-date on their cancer screenings. However, kids that get this disease do not have an increased risk of cancer.
Skin care for scleroderma and dermatomyositis
It is important to follow the recommendations of your treating doctor. In my practice, I always recommend:
- a hypoallergenic gentle and hydrating skin care routine and,
- a really good broad spectrum sun screen and sun protection.
I recommend the same products that I mentioned above for lupus:
Scleroderma and dermatomyositis, like lupus cause rashes that damage and weaken the skin barrier making it imperative that you avoid harsh skin care products and allergens. You also want to help skin heal using deeply hydrating products. In my practice, I would create a skin care routine like this:
Cleanse skin using only a gentle fragrance-free pH balanced cleanser like VaniCream Cleansing Bar
After all skin cleansing, I would recommend my patients apply a fragrance-free deeply hydrating moisturizer such as my Natural Face and Body Lotion within 3 minutes after cleansing skin and toweling off the excess water. This hydrating step helps skin barrier heal. Know that dry skin is injured skin and will be slower to heal.
 I would have them take extra care with their hands, which need to be washed many times during the day to prevent infection. This means keeping a good hand cream in a convenient location, such as at every sink to apply after washing. My preference is a product like my Dry Skin Hand Repair Cream is fragrance-free, non-greasy and the ideal dermatologist-recommended hand cream.
I would have them take extra care with their hands, which need to be washed many times during the day to prevent infection. This means keeping a good hand cream in a convenient location, such as at every sink to apply after washing. My preference is a product like my Dry Skin Hand Repair Cream is fragrance-free, non-greasy and the ideal dermatologist-recommended hand cream.
 It is important not to forget the delicate lip skin. I recommend that my patients get in the habit of using a flavor and fragrance-free lip balm to prevent chapped lips such as my Natural Lip Balm. When in the sun, use a mineral SPF lip balm.
It is important not to forget the delicate lip skin. I recommend that my patients get in the habit of using a flavor and fragrance-free lip balm to prevent chapped lips such as my Natural Lip Balm. When in the sun, use a mineral SPF lip balm.
Every day it is important to apply a pure mineral broad spectrum SPF 30+ sunscreen to all exposed skin. Remember that UVA comes through windows and all UV rays can bounce into shade. Use UPF 50 clothing to sun protect as much skin as possible and always wear a UPF 50 sun hat with a 3+ inch full circumference brim when outside. Be sure that your hat also covers the top of your head.
Click here to see my broad spectrum mineral zinc oxide sunscreens.
The bottom line with autoimmune diseases and your skin:
Your skin is your body's biggest organ and you can easily examine it yourself. Some internal health problems, including many autoimmune conditions, have signs that show up on your skin. If you develop unusual skin problems, it's advisable to see a dermatologist. Dermatologists are the medical experts for skin conditions; a dermatologist is the best medical professional to evaluate cutaneous manifestations of internal disease.
Disclaimer: The information in the Dr. Bailey Skin Care web site, and related links, articles, newsletters and blogs, is provided for general information and educational purposes only. It is the opinion of Dr. Cynthia Bailey, or other indicated authors. Consult your physician or health care provider for any specific medical conditions or concerns you may have. (This also applies to patients in her medical practice; the information here is not a substitute for, or an extension of, the medical care she provides for you.) Never disregard professional medical advice or delay seeking it because of something you have read here. Use the information and products on this site at your own risk. Use of this site indicates your agreement with these statements and the Terms and Conditions of DrBaileySkinCare.com. If you do not agree to all of these Terms and Conditions of use, please do not use this site!
