Melanoma - What is it?
By Cynthia Bailey MD.

Melanoma - what is it, how is it different from other skin cancers and how do you tell if one of your moles is worrisome for being a melanoma? As a dermatologist who has specialized in skin cancer for over 35 years, and done over 200,000 skin exams on Californians, I've learned how to explain melanoma to my patients in a way that makes the topic clear. This is important information and you need to understand what melanoma is and how to watch for it on your skin and the skin of those you love.
How is melanoma different from other skin cancers?
Melanoma is a cancerous growth of the cells in the skin called melanocytes. These cells are normally sprinkled among the more numerous skin cells called keratinocytes in the top living cell layer of your skin called the epidermis. Melanocytes are the only cells that produce melanin pigment, which creates your skin color and a tan. These same cells are what moles are made of. In moles, melanocytes are clumped into bunches (called nests) in the epidermis, dermis (second living layer of skin), and even reaching down into the fat layer below the dermis (subcutis).
Melanocytes are not the main cells that make up the epidermis. The epidermis is made up of layers of cells called squamous keratinocytes and basal keratinocytes. Keratinocytes can also become cancerous. These cancers are called Basal Cell Carcinoma and Squamous Cell Carcinoma. Precancerous growths of keratinocytes are called Actinic Keratosis.
The distinction between keratinocytes and melanocytes is important because their cancers are entirely different – like apples and bananas. They are unrelated and one does not become the other. The information in this article is specific for melanoma.
What are melanocytes?
Melanocytes scattered sparsely between keratinocytes in the epidermis of your skin. They are clumped in nests in your moles. Melanocytes are also present in the central nervous system (spine, brain, and eyes), inner ear, and the heart. Melanoma cancer is caused when one of these cells mutates and grows uncontrollably into a tumor that can spread to distant sites in the body.
UV rays are one of the significant causes of melanocyte cell mutation.

UV ray exposure is also preventable. Melanoma is deadly and the occurrences are increasing. It can even affect children and young adults. If not caught early, it will spread through the body. As a dermatologist, I am passionately dedicated to preventing melanoma on the skin and catching it early. This mission saves lives. As part of this personal mission, I educate people on UV ray skin exposure and early detection of melanoma. The cancer is much less likely to be deadly, and treatment is easier and more successful, in the early stages of melanoma. Everyone needs to learn how to recognize melanoma on their skin. Everyone also needs to know how to protect their skin from UV ray damage.
How to know if you are at high risk for melanoma
You are more likely to get melanoma if you:- have fair skin, especially if you or your parents have red hair or are blond and/or have blue green eyes,
- have a history of blistering sunburns. 5 or more sunburns between ages 15-20 increases your risk by 80%,
- have many moles or if your moles are large and irregular (dysplastic nevi),
- have a history of unprotected sun exposure,
- have used a tanning bed,
- have a relative who has had melanoma, and
- are in the upper middle-class (curious, right?!).
Dermatologist explains how to examine your skin for melanoma
Whether you are at high risk or not, do monthly self-skin exams to keep an inventory of your ‘spot collection’. It’s best done with a mirror.
The goal is to get a general impression of your spots and be certain they are not changing. Spouses, partners, and parents may be needed to help examine your back.
Screen your skin for melanoma
We teach you to look for these 5 worrisome signs: ABCDE’s of Melanoma.

What are the ABCDE signs of melanoma?
A: Asymmetry
- This refers to when moles are irregularly shaped - not round or oval.
B: Border
- A melanoma sign is when the mole’s edges are jagged, blends into skin, notched, or scalloped.
C: Color
- Be wary when the color throughout a mole is not uniform.
D: Diameter
- Measure if the diameter of a mole is greater than 6 mm (approximately the size of a pencil eraser).
- You may identify melanomas smaller than 6 mm.
E: Evolving over Time
- Examine if the mole is raised or not flush with your skin.
- Does the mole become tender or ulcerate?
- Does the mole itch?
- Is it growing?
- Watch if the mole changes over time in size or color (darker, lighter, red, blue, black, white and even shrinking – it all counts).
What is the Ugly Duckling Sign of melanoma?
The Ugly Duckling Sign is a mole that does not match your other moles. For example, your moles may be light brown with an exception of a black mole. That would need to be evaluated by an expert during your full skin exam. Other odd patterns may be your moles are all dark and one is lighter, red, or has a white circle around it.
When it comes to catching melanoma I like to say, "when in doubt, check it out!" Schedule an appointment with a Board-Certified Dermatologist if you suspect one of the moles on your body may be melanoma. A full skin exam is painless and I can’t tell you how many times a patient has saved their life by scheduling one! Catching melanoma early can make this scary diagnosis a lot less scary.
Do All Melanomas Come from Moles?
The surprising answer is no! In a vital scientific study, it was found that,
only one-third of melanomas arise from existing moles!
The vast majority of melanoma cancers appear on the skin as new spots according to the study published in the Journal of the American Academy of Dermatology. These investigators reviewed 38 published studies comprising 20,126 melanomas. They found that less than one-third of melanomas (29%) arose from an existing mole. The vast majority (71%) appeared as new spots. Melanomas that arose from existing moles were thinner, indicating that patients whose melanoma was associated with an established mole had a better prognosis. We don’t know why this is.
Melanoma Identification – Practical Examples
Here are two examples of how to identify melanoma using the ABCDE’s of melanoma.
Melanoma #1: Notice in the picture that it is,
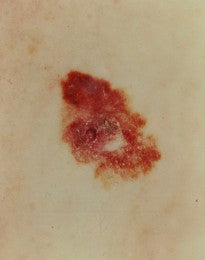
- A: Not perfectly oval.
- B: Poorly-defined margins. Some margins are very dark, while others are light and blend into the skin
- C: Color not uniform. Dark red in some areas, lighter in others. White area in the center.
- D: It is larger than a pencil eraser.
- E: The lesion is changing and has been growing, scabbing and scaling, and even going away in the center.

Melanoma #2: Notice in this image that the spot is,
- A: Asymmetrical. No clear shape.
- B: Border clearly defined but ragged. Scalloped in some areas.
- C: Distinct color variations. A dark reddish-purple to black border outlines the mole with a white center that is also paler than the regular skin tone.
- D: It is larger than a pencil eraser.
- E: The lesion is spreading out and seems to be losing color in the center.
What Contributing Factors Increase the Risk of Melanoma?
1. UV ray exposure of skin increases the risk of melanoma.
We know UV rays damage DNA. Both regular and intermittent exposure to the sun contributes to sunburns and melanoma. Damaged DNA sometimes “turns on” an oncogene (a gene that causes a tumor cell) or “turns off” a tumor suppressor gene (a gene that usually stops the uninhibited growth of cells), which opens the door for cancer to develop. It’s essential to protect from UV damage by wearing a really good broad spectrum sunscreen every day on all exposed skin.
2. Geography of where you live may increase your risk of getting melanoma.
Since UV rays damage DNA, it makes sense that more intense sun would cause more severe damage. People who live close to the equator as well as those living at high altitudes get more intense sun exposure and have an increased risk of melanoma.
3. Having a family history of melanoma will increase your risk of getting melanoma.
Melanoma can be labeled “familial” when two or more first-degree relatives have had melanoma. When there are alterations in one of two specific genes (named CDKN2A or CDK4), people are at risk for this type of melanoma. Individuals with familial melanoma often have “funny looking moles” which is known as “atypical mole syndrome,” a condition in which moles may appear irregular looking and are sometimes difficult to visually distinguish from melanoma. When melanoma runs in your family or you have many unusual looking moles, it is critical to see a board-certified dermatologist for regular skin checks.
4. Having a lot of moles and freckles may mean you have a higher risk of getting melanoma.
Having many moles increases the risk of developing melanoma. Over 100 moles can increase your risk 10x. Having lots of freckles is also a risk factor.
5. Your skin type tells you a lot about your risk of getting melanoma.
Melanoma is more common in Caucasians, particularly in fair-skinned people. Redheads with light eyes seem particularly susceptible. This does not mean that darker-skinned people can’t get melanoma, but it is less common. Everyone is at risk of getting melanoma but really fair Caucasians and redheads are particularly prone. Even just having a gene for red hair but not being a redhead can increase your risk. Click her to learn more if there are people with red hair in your family.
What's the bottom line with melanoma skin cancer?
Anyone can develop skin cancer, including melanoma. 1 in 50 Americans are estimated to develop melanoma during their lifetime.- Melanoma is caused mainly by intense, occasional UV exposure (frequently leading to sunburn), especially in those who are genetically predisposed to the disease.
- It kills an estimated 9,940 people in the US annually; one person dies of melanoma every hour (every 57 minutes).
- It is not the most common of the skin cancers but it causes the most deaths.
- Melanoma is one of only three cancers with an increasing mortality rate for men, along with liver cancer and esophageal cancer.
- Women aged 39 and under have a higher probability of developing melanoma than any other cancer except breast cancer.
- Each person with a first-degree relative diagnosed with melanoma has a 50 percent greater chance of developing the disease than people who do not have a family history of the disease.
Dermatologist's 6 Education and Patient Care Tips for Melanoma
- My job as a dermatologist is to help prevent melanoma and to detect it early. I perform full body skin exams. In patients who are at high risk for melanoma, I recommend an annual full body skin exam.&
- New moles after the age of 30 need to be given attention as does any changes in existing moles. I teach people that most melanoma comes from new moles though a change in an existing mole is also important.
- I teach patients to do monthly self-exams and become familiar with their general inventory of moles. This includes scalp, between toes etc. For the back, enlist the help of a loved ones.
- When a person has more moles than I can document on a written map, I capture total mole map photos and compare them during exams. I recommend that my patients do the same and use the images for their self-exams.
- I teach patients the ABCDE foundation of assessing their moles and the Ugly Duckling Sign. During their exam, I help my patients recognize their general pattern of moles and how to distinguish their moles from the other spots on their skin.
- If a mole itches, develops a white halo, or turns into a scab or sore, I stress the importance that they come show me the spot.
It is comforting to have a strategy and a healthy amount of suspicion when it comes to detecting melanoma in an early and more easily curable stages. Pay attention to even a tiny change in your moles. In my years of dermatology practice, I have had patients detect their own melanoma simply because of an itch in, or a hunch about, a mole. Because early detection is lifesaving, an open-mind during skin exams is essential. If your doctor dismisses a mole you are worried about, you may be well served to get a second opinion.
Explore Further
I also educate my patients about effective sun protection techniques. Being outside is a pleasure and doing it without UV mutation is possible. Read the following guides and articles. These tips are practical and have been refined by my patients and I over 30 years. We know how to enjoy the sun minus the UV skin damage.
